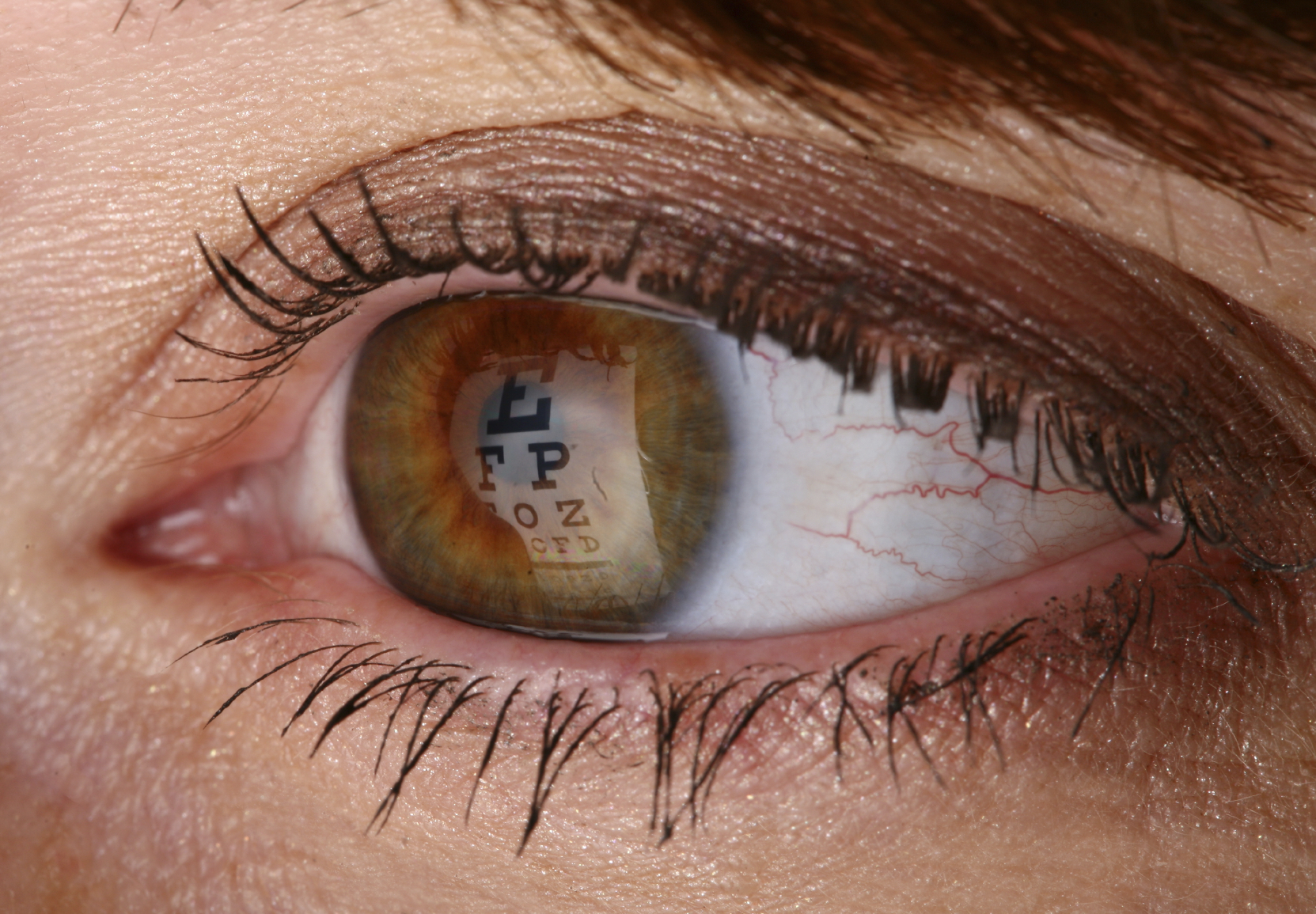
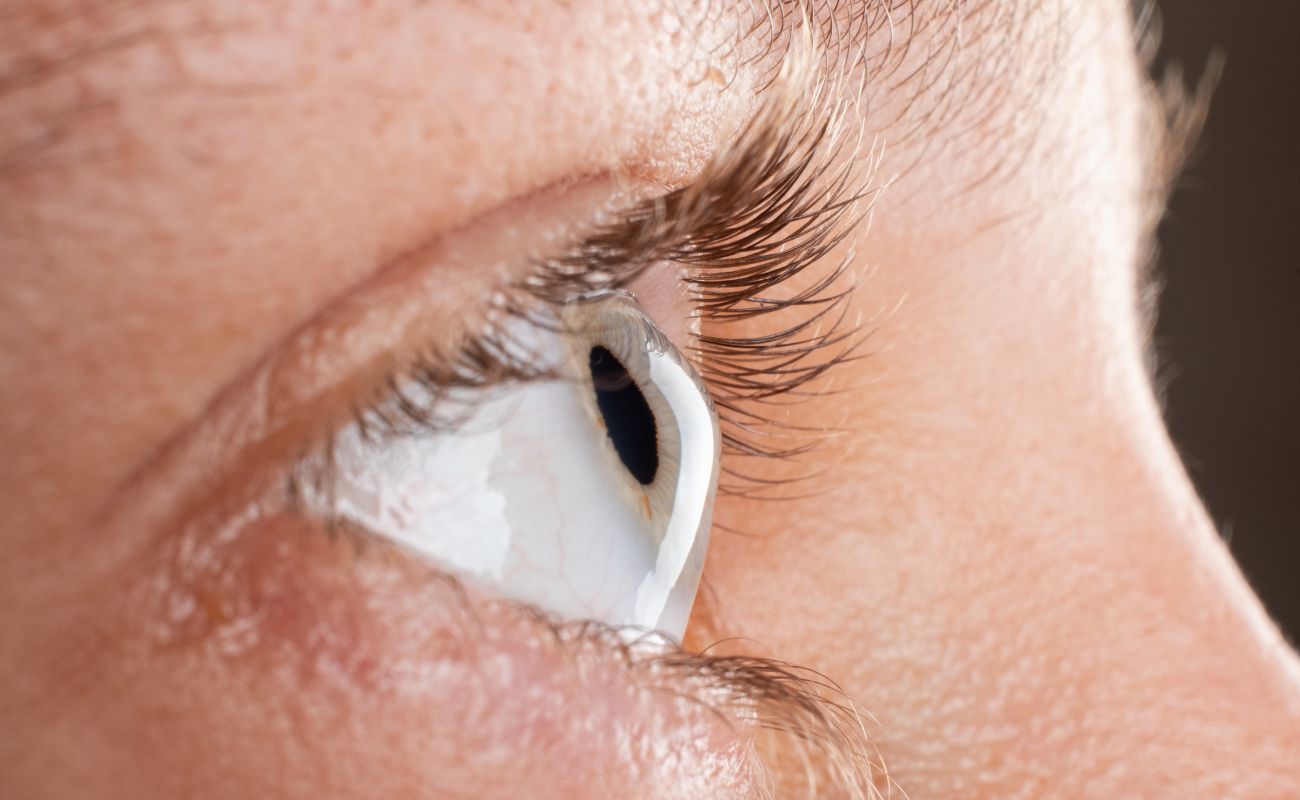
Are you worried that you or a loved one has developed keratoconus? If so, your first step should be to make an appointment with a trusted optometrist. Keratoconus is a condition where the cornea, the eye’s outermost layer and lens, starts to become irregular and bow forward. Since the cornea plays a crucial role in controlling the quality of light that gets into your eye—and focusing that light onto the retina, so that your brain can properly process visual information—any shape change or weakening of this surface can result in significant vision disruption. Specifically, if you are experiencing keratoconus, you will notice that your vision gets blurrier over time. Most patients with keratoconus develop the condition in their teens or twenties and then experience a progression of irregular astigmatism (the refractive error that keratoconus causes, where the cornea is not focusing light evenly on the retina) over a decade or more.Symptoms of Keratoconus Keratoconus is not the only eye condition that results in astigmatism. In fact, astigmatism occurs as a result of many irregularities in the cornea's shape that prevents light from focusing directly onto the retina. As such, the symptoms that keratoconus brings about—blurry vision, distortion, glare, eye strain, headaches, etc.—are the same symptoms you would likely experience with any underlying cause for irregular astigmatism. How do you know whether the root of the issue is keratoconus? Again, your first step should be to see an eye care practitioner and undergo a thorough eye exam.In keratoconus, the weakening of the cornea ultimately causes the corneal surface to become thinner and thinner over time. Eventually, the cornea becomes so weak that it can no longer match the eyeball's spherical shape and starts to bulge outward in a cone-like shape (hence the name “keratoconus”). The more conical the cornea becomes, the more severe the symptoms will become, ranging from nearsightedness to extreme glare around lights and visual distortion—particularly in nighttime or low-light conditions. One symptom patients won’t experience is pain: though many people diagnosed with keratoconus assume that the bulging of the cornea will be painful, pain is not a common symptom.Getting Diagnosed for KeratoconusThere are several methods that an eye care practitioner can use to diagnose keratoconus, beyond asking the patient about symptoms or noticing a conical corneal shape as part of a basic eye exam. One strategy your eye doctor may try is a refractive eye exam. The optometrist uses a device called a retinoscope with a phoropter to test how effectively different lenses are for correcting your vision issues. This test is useful for diagnosing any refractive error, including myopia (nearsightedness), hyperopia (farsightedness), astigmatism, or presbyopia (age-related farsightedness) but can help diagnose keratoconus due to the unique way light reflects in this condition.Other tactics include slit-lamp exams, keratometry tests, and corneal mapping (corneal topography). In a slit-lamp exam, your eye doctor will use a beam of light and a microscope to examine your eye, including the shape of your cornea. This method can be useful to spot early thinning of the cornea. In a keratometry, an eye doctor directs a circle of light onto the surface of your cornea and uses the reflection of the light to assess your corneal curvature. Finally, in corneal mapping or topography, your optometrist will use photographic technology to record images of your cornea and assemble topographic maps of the corneal surface. This computerized mapping process is terrific for ascertaining corneal thickness, irregularities in cornea shape, and early signs of keratoconus.Visit Miami Contact Lens Institute Today At Miami Contact Lens Institute, we not only can diagnose keratoconus cases, but we are also experienced at implementing effective keratoconus treatments. Our definitive, go-to treatment for keratoconus is to use scleral lenses, custom-designed contact lenses that rest on the white of the eye (the sclera) and then vault over the corneal surface. This design, which protects the ocular surface by leaving a tear-filled chamber between the eye and the contact lens, helps compensate for irregularities in corneal shape, including irregularities caused by keratoconus. Our experience has been the scleral lenses are the best option for providing comfort and clear, stable vision for patients with keratoconus.

Relevant post: Ten Questions to Ask Your Optometrist about Scleral LensesTo learn more about keratoconus, keratoconus diagnosis, and keratoconus treatment, contact us today.[embed]https://youtu.be/-3rcavKnT_U[/embed]Testimonial from Shahin, a Miami Contact Lens Institute's patient I had an excellent experience with Dr. Kramer, having suffered from significant Keratoconus in my right eye. The scleral lenses, which were new to me, also greatly aided my night driving and overall vision. Dr. Kramer was very professional and thorough during the entire process. Highly recommend.